PATIENT INFORMATION SHEET
Raynaud’s Phenomenon
What is it?
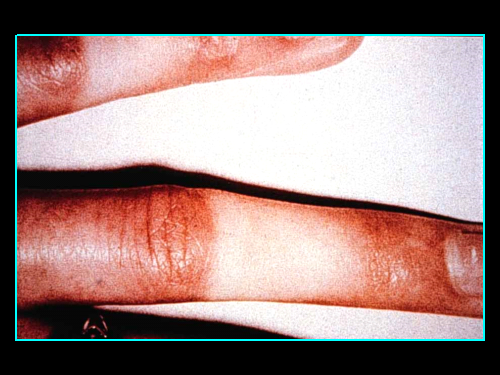
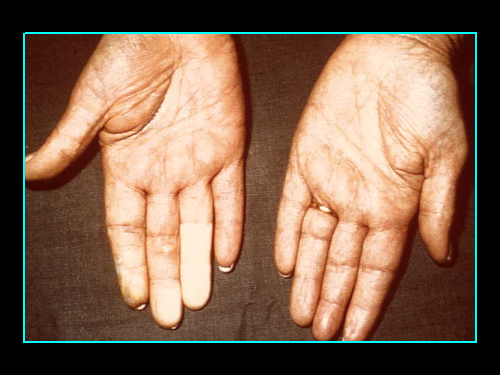
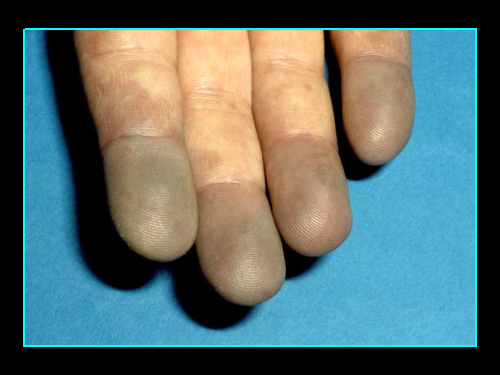
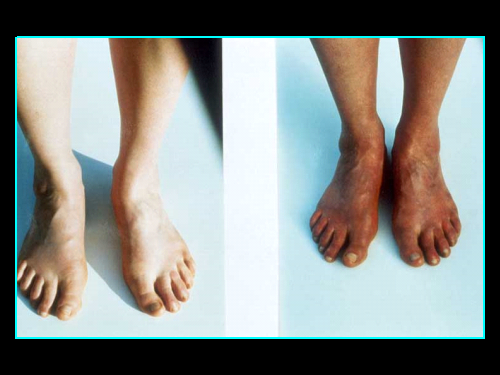
Raynaud’s Phenomenon is the name given to the condition in which the affected part of the body, usually the hands and feet, become cold, numb and often painful. The hands or feet may undergo three different colour changes – white, then blue, then red. Some people only experience the white colour change (blanching), and it is not necessary for a diagnosis of Raynaud’s to experience all three colour changes.
The symptoms are caused by constriction of the blood vessels which normally supply the extremities, usually the hands and feet, particularly the fingers and toes. On exposure to the cold, or with changes in temperature or strong emotions such as stress, these small blood vessels go into spasm and temporarily prevent the blood flowing. This lack of blood turns the fingers and toes white and numb, and sometimes painful.
The bluish colour occurs when the blood that is trapped in these vessels becomes deoxygenated (the oxygen is removed by the tissues). When blood is deoxygenated it changes from a red colour to blue. The final stage is a red discolouration and occurs when chemicals are released from the lining of the blood vessels. These chemicals cause the blood vessels to vasodilate (open up) and fresh red blood rushes in to the affected area. This is often accompanied by tingling, burning and even pain.
Although, Raynaud’s affecting the fingers and toes is the most common, it can also affect the tip of the nose, the lips and ears. Also, although cold is the most common cause, pressure can also cause Raynaud’s and patients may notice their fingers going white when carrying, for example, shopping bags.
Why the name?
Raynaud’s Phenomenon received its name from a French doctor, Maurice Raynaud who first described the condition in 1862. Since Maurice Raynaud’s discovery, a lot of research has gone into what is causing Raynaud’s and much more is now known about the condition. It is very common and varies in severity from mild to severe, where it has life changing effects.
Primary or Secondary Raynaud’s Phenomenon?
Primary Raynaud’s Phenomenon affects about 20% of young women. It is not really a disease but actually an exaggerated response to cold. The above symptoms occur when the patient is exposed to the cold, changes in temperature, strong emotion or pressure. Although, it can be very troubling indeed, necessitating an almost hermit like existence in the winter, it does not progress and skin damage causing ulcers does not occur. It is often associated with migraine headache, irritable bowel syndrome, and may run in families.
Secondary Raynaud’s Phenomenon is where the Raynaud’s occurs along with an ‘associated disorder’. The associated disorder is often a rheumatological disease such as one of the connective tissue disorders. These include Systemic Sclerosis, Systemic Lupus Erythematosus, Mixed Connective Tissue Disease, Sjogren’s Syndrome and Rheumatoid Arthritis. This form of Raynaud’s can be severe and associated with finger ulcers, although this latter is becoming increasingly rare due to more effective treatments becoming available.
There are other forms of associated disease leading to Raynaud’s such as Hand Arm Vibration Syndrome where the patient has been exposed to vibrating machines, often hand-held air driven tools such as road drills.
Some medications can also bring on Raynaud’s and if you have developed Raynaud’s after starting a new drug, it would be worthwhile discussing this with your own doctor. Other disorders, such as an underactive thyroid are also associated with secondary Raynaud’s.
Treatment
As a lot of Raynaud’s sufferers are young women, a non-drug approach is the best first step. There are many aids that can help cold fingers and toes. These include battery heated gloves, hand warmers, etc. Learning how to manage Raynaud’s is also helpful and this includes putting on gloves before going outside (cold fingers that are already cold will not heat up), putting on gloves before taking items out of the freezer, wearing a hat and vest, persuading others to do the washing up, particularly if the water is cold!
Drug Treatment of Raynaud’s
Nearly all of the medications used in the treatment of Raynaud’s dilate up the blood vessels in the fingers and toes. Some can be very effective but there is no way to tell whether a patient will respond better to one drug than another, and so often trial and error is required. As all these drugs open up the blood vessels, it is unsurprising to note that the side effects are related to this. It is impossible to have a drug that merely dilates the blood vessels of the fingers and toes, and they often dilate elsewhere for example, producing headache, facial flushing and swelling of the ankles. Side effects can be avoided by very slowly increasing the dose of a medication, or by remaining on a low dose. There are a number of different drugs within the same family, and a number of different families of drugs which have been shown to help Raynaud’s. If you have Raynaud’s, you should discuss these with your own doctor.
Conclusion
Raynaud’s is a very common disorder and it can be extremely troublesome. Often a patient looks well so it is difficult for others to understand how seriously this condition can affect life. When a secondary Raynaud’s Phenomenon is discovered, the patient also has the signs and symptoms of the associated disease and finger and toe ulcers mean doing anything with the hands and feet can be difficult and painful. Despite the severity of the condition, there are medications and lifestyle changes that can help significantly. Do not be afraid to go along and discuss these with your own doctor, who will recognise that Raynaud’s Phenomenon can be a very troublesome disorder and advise what is best for you.
Systemic sclerosis:
https://www.arthritisresearchuk.org/arthritis-information/conditions/systemic-sclerosis.aspx
Systemic Lupus Erythematosus:
https://www.arthritisresearchuk.org/arthritis-information/conditions/lupus.aspx
Sjogrens Syndrome:
https://www.arthritisresearchuk.org/arthritis-information/conditions/sjorgens-syndrome.aspx
Rheumatoid Arthritis:
https://www.arthritisresearchuk.org/arthritis-information/conditions/rheumatoid-arthritis.aspx
Author: Professor Jill Belch